Diabetic retinopathy is the name given to the changes in the retina which occur over a period of time in diabetics. The extent of these changes determines what type of diabetic retinopathy you have.
Typically, diabetes damages the fine network of blood vessels that supply oxygen and nutrients to the retina. When these blood vessels become blocked, leaky or grow abnormally, resulting in bleeding and scarring, the retina becomes damaged and is unable to work properly reducing vision.
Diabetic retinopathy is a potentially blinding disease, but most sight loss from diabetic retinopathy can be prevented with early detection, monitoring and appropriate treatment of the retinopathy. Good control of blood sugar, blood pressure and blood lipids also reduce the risk of developing sight-threatening retinopathy.
In its early stages, there may be little or no visual symptoms. Without early detection and treatment, Diabetic Retinopathy can permanently damage the retina. If the condition is not caught early, it may produce symptoms that affect vision.
These include mild blurriness in near, or distance vision, floaters and even the sudden loss of vision. If left untreated, it can cause severe vision loss, and even blindness. Eye surgeons cannot reverse the damage caused by Diabetic Retinopathy, but if caught in time, modern treatment options may help slow its progression, and prevent further vision loss.
It is critical for patients with diabetes to be examined on a regular basis, even if they have not yet noticed any symptoms. If a patient experiences any significant change in their vision, they should contact their doctor for an immediate appointment, even if they recently had an examination.
Non-proliferative or background diabetic retinopathy
This is the most common type of diabetic retinopathy and many people who have had diabetes for some time will have this early type. The blood vessels in the retina are only very mildly affected. As long as the macula is not affected, vision is normal and you will not be aware anything is wrong. Over time, the swelling, or edema, thickens the retina causing the vision to become blurred.
Maculopathy
Maculopathy means that your macula is affected by retinopathy. If this happens, your central vision will be affected and you may find it difficult to see detail such as recognising people’s faces in the distance or seeing detail such as small print. Most maculopathy can be treated with laser with the aim of preserving as much vision as possible.
Proliferative
Once the disease reaches the more advanced proliferative stage, it can cause larger blood vessels in the retina to become blocked. These blockages can result in areas of the retina becoming starved of oxygen, known as ‘ischaemia’. If this happens the eye is stimulated into growing new vessels, a process called ‘neo-vascularisation’; which is nature’s way of trying to repair the damage by growing a new blood supply to the oxygen starved area of your retina.
Unfortunately, these new blood vessels are weak, and grow in the wrong place – on the surface of the retina and into the vitreous gel. As a result, these blood vessels can bleed very easily which may result in large haemorrhages over the surface of the retina or into the vitreous gel.
Extensive haemorrhages can lead to scar tissue forming which pulls and distorts the retina. This type of advanced diabetic eye disease can result in the retina becoming detached with the risk of serious sight loss.
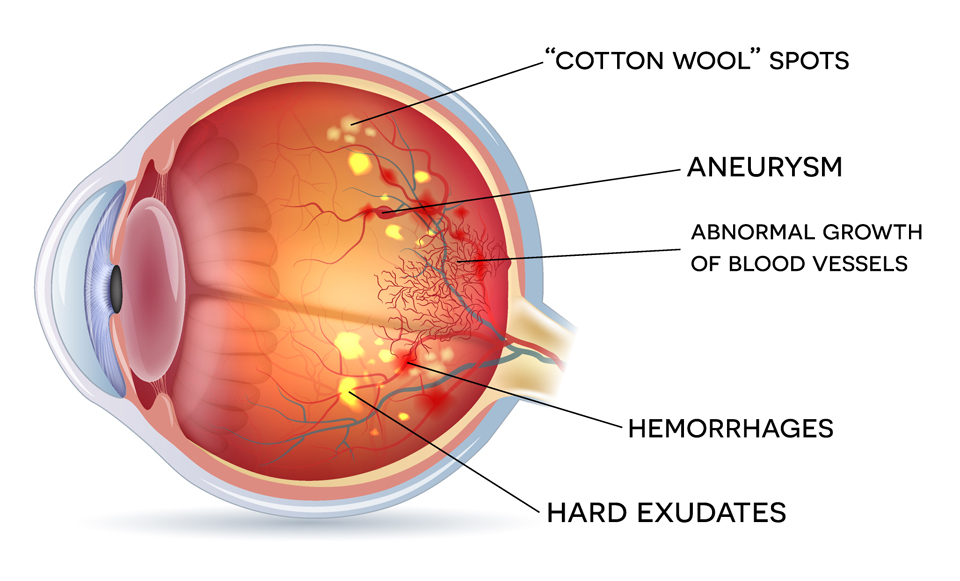
In its early stages, diabetic retinopathy may not affect your vision, and you may not even be aware that you have it.
Therefore it is important to have regular check-ups from an eye specialist if you suffer from diabetes.
When diabetic retinopathy starts to affect your vision, you may notice you have difficulty with reading and close-up work as a result of leaky or blocked blood vessels in the macula, which is the centre of the retina (maculopathy). The macula is the most used area of the retina, providing our central vision and is essential for clear and detailed vision. Floaters and double vision may also be symptoms of diabetic retinopathy; although they can have other causes too.
If your vision is getting worse it does not necessarily mean you have diabetic retinopathy. Your vision can become blurred whilst your diabetes is being controlled. This could be due to temporary changes in the lens of the eye whilst the diabetes is being stabilised. Diabetes can also make you especially prone to developing early cataracts affecting vision.
Did You Know?
Within 20 years of diagnosis nearly all people with Type 1 Diabetes and two-thirds of those with Type 2 Diabetes are likely to have diabetic retinopathy.
High blood sugar levels can cause damage to the blood vessels in your retina (the focusing surface at the back of your eye). When damaged, these blood vessels can leak fluid or bleed, which causes the retina to swell and form deposits, resulting in blurred vision.
People with diabetes are at most risk from retinopathy, and the longer you have diabetes, the higher the risk.
Hypertension, smoking and pregnancy can also increase your risk of developing diabetic retinopathy.
You may think that systemic hypertension, better known as chronic high blood pressure, only affects your heart and kidneys, but did you know that it also can cause serious vision problems if left untreated?
Increased pressure causes the walls of your blood vessels to thicken. This reduces the amount of space in your blood vessels, making it harder for blood to reach the retina in the back of your eye where images are focused. This is called hypertensive retinopathy, which can impair your eyesight.
If you begin to see changes in your vision such as decreased eyesight, double vision, or even blind spots accompanied by headaches, it is important to talk to your eye care professional immediately. To diagnose hypertensive retinopathy, he or she will assess any damage to your retina by looking for narrowed blood vessels or signs of leakage.
The early stages of hypertensive retinopathy might not show any symptoms. Therefore, it is important to diagnose and treat your high blood pressure as soon as possible to avoid any damage to your eyes or other organs. High blood pressure can often be managed and even prevented through routine blood pressure monitoring and lifestyle changes. If you have or are at risk of developing hypertension, talk to your primary care physician today to control your high blood pressure and protect your eyesight.
As soon as you are diagnosed with diabetes, you should make an appointment for a diabetic retinopathy check-up.
If you do have diabetic retinopathy, your treatment will depend on the stage of the disease.
In the early stages: diabetic retinopathy needs regular monitoring rather than treatment. Laser (laser retinal photocoagulation) is the principal treatment for diabetic retinopathy.
Maculopathy: laser treatment for maculopathy is used to deal with leaks from blood vessels. However, diffuse diabetic maculopathy may respond relatively poorly to laser treatment and injections into the eye may be more effective at stabilising or improving vision on their own or in combination with laser treatment.
Proliferative diabetic retinopathy: can be treated with laser to remove the stimulus for the growth of new blood vessels (which replace the blocked and damaged vessels); alongside other new treatments which can provide useful adjuncts to stabilise vision.
If you experience any of the above symptoms or would like some advice regarding diabetic retinopathy treatment please call us on 01392 699969 or book a consultation.
Copyright © 2026 All Rights Reserved | Privacy & Cookies | Accessibility | Translate | website by: www.onebrightspark.co.uk